
This exhibit contains selected footage from video-based interviews conducted as part of the National Humanities Center’s COVID-19 Oral History Project alongside research posters and written reflections produced by medical students at Duke University and the University of Washington, who acted as interviewers for the project. Together, this material sheds light on the ways that the humanities are enriching medical education today and allowing the clinicians of the future to engage deeply with their professional communities, respond to structural forms of inequity, and prepare for new challenges of caring.
Exhibit created by Jane McGrail, Head of Community Engagement and Outreach, NHC COVID-19 Oral History Project.
Kevin Glover, University of Washington
“I have heard several commentators talk about how they think COVID-19 has fundamentally reshaped the healthcare profession in the United States, but I had only tangentially experienced that during my pre-clinical years of medical school. We were safely cloistered away in our books, without any responsibilities for patient care. When I conducted these interviews, I was on my first clinical rotation and I was starting to work alongside healthcare professionals who had been shouldering the weight of their community’s healthcare needs for more than a year and a half. They seemed tired.
“By doing these oral histories, I was given a deeper look into how these professionals were feeling about their work. There was a real sense of permanent change, but not necessarily about how healthcare is delivered. It seemed like the relationship between these providers and their communities had changed; I remember one public health professional telling me, ‘we’re all just so disappointed with our community.’ It seemed like the values of these professionals—saving lives, promoting wellbeing—weren’t necessarily shared by their rural community members.
“That might sound hard or harsh, and perhaps it is. And there are many stories of solidarity, strength and human perseverance that will brighten recollections of this time. But for my respondents, there was a new rupture between healthcare providers and rough-and-ready, individualistic community members. It seems like my generation of physicians will be working to rebuild trust with these people, or risk alienating them from the healthcare system entirely.”


Nitika Gupta, University of Washington
“After a year of slogging through pre-recorded lectures and Zoom class, I (like many of my classmates) struggled to remember why I chose to pursue medicine; after all, my passion for human connection far surpassed my interest in pathophysiology of disease. Completing the oral history project was a welcomed change, as it allowed me to learn from human stories rather than 2-dimensional screens.
“Like many federally qualified health centers, the International District Medical and Dental Clinic is quick-paced; my preceptors often speed-walked from room to room to ensure that each patient received adequate time. I appreciated the oral history project because it allowed me to slow down and understand the spirit behind the hard-working ICHS staff, as well as connect with team members that I otherwise may not have met.
“Before ICHS, my career goals felt nebulous. I dreamt of offering accessible, justice-centered care but didn’t know how to bring that dream to fruition. Listening to ICHS staff share their experiences of working during the COVID-19 pandemic was empowering; it reaffirmed my commitment to medicine and clarified my goals for the future. I can’t wait to work alongside a team of diverse, compassionate staff to provide care that meets patients where they’re at.”
Megha Gupta, Duke University
“In participating in this project, I had the privilege of interviewing four people in very different healthcare settings, each with highly individual and intense experiences as leaders and care providers during the pandemic. They faced realities of racism, fragile healthcare structures, and their own vulnerabilities with family and community. In conducting these interviews, I realized how exposed healthcare workers are, and how difficult it can be to operate even with the protections of an academic medical center. In taking my next steps in my journey as a physician, these interviews helped me learn to honor the stories of my colleagues and the difficulties they face.
“I was also able to deeply connect based on my own experiences as a student throughout the early years of the pandemic. I remember feeling very impotent in those moments—not knowing if I would unwittingly infect others, feeling like I left my patients behind, doing my best to get folks vaccinated, and fearing for my loved ones, much as my interviewees had felt. Moving forward, I hope to create environments where we share both the joys and inevitable grief that medicine endures. This project highlighted how much our community needs space to be vulnerable, and that the monolith of a perfect, industrialized, machine-like academic medicine doesn’t always provide that. Working to change this culture will certainly be a group effort, but I’m so happy to have been a part of people sharing the stories and taking the first steps to initiate these long overdue changes.”


Fred Heller, Duke University
“I found a lot of value in participating in the COVID-19 Oral History Project. For one thing, participating in the project was a great outlet for connection. As a medical student, I’m steeped in healthcare environments, but I never had the opportunity to delve deep into the experience of COVID with other professionals around the hospital. I felt less isolated after conducting a few interviews, even when my experiences or feelings differed from those I interviewed. The sense of connection I felt extended throughout the process; brainstorming questions and being trained to take an oral history alongside classmates was an excellent way to connect without tiptoeing around the elephant in the Zoom room.
“Another benefit was that participation in the project allowed me to feel active. As a medical student, I’d been barred from participating in care of COVID patients for most of the pandemic. The chance to take an active role in preserving the experiences of healthcare workers was something tangible I could contribute. I also saw how the opportunity to share their stories was cathartic for the workers whom I interviewed, and so felt like giving that outlet was a further contribution.
“Finally, I practiced many interview skills while taking histories. Skills like asking open-ended questions, communicating respect and appreciation, and allowing for silences. These are directly applicable to the way I want to interact with my patients as I transition to residency, and I was grateful to have the opportunity to further hone them.”

Nick Johnson, University of Washington
“The thought of public speaking or doing an interview is enough to get the nerves jumping in me. At the same time, I’ve always found that my best personal and professional growth happens at the edge of my comfort zone. When I became involved with the oral history project for my summer medical school experience, I knew that it would be a way for me to get to know my clerkship community better and to grow.
“Doing one-on-one oral history interviews was something completely new to me, so thankfully we had training on what to do and expect and great examples to follow. I found those nerves bubbling up when I would go to meet new people to interview, and I also found my understanding of the connections within the community deepened. As each interview progressed, I became more comfortable asking questions and active listening to bring each person’s story to the surface.
“Being able to listen well and ask the right questions is an important skill to develop as a healthcare provider, and I found that participating in this project gave me the right kind of practice to build those skills. Listening to each person and how COVID impacted their life and their community shifted my perspective and made me think of the greater impact of the pandemic. Medical humanities opened me up to see the world through the point of view of other people, and I believe that sharing our stories with each other is a wonderful way to build connection and community.”

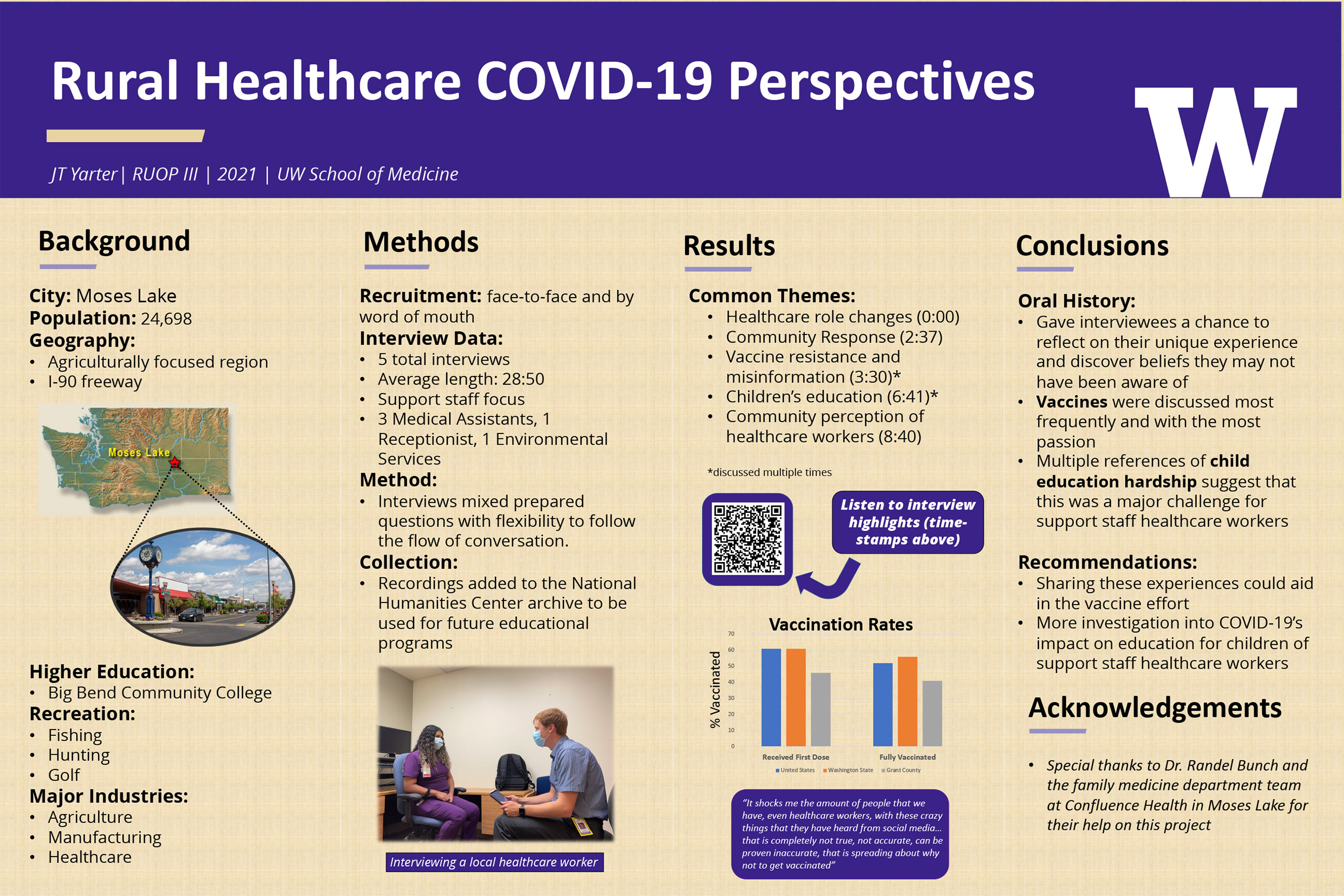
Sophia Orlando, University of Washington
“I have grown to understand hospitals and their employees as a community. Through the four interviews I conducted as part of the oral history project, I heard firsthand how each member of the larger team contributed to the health and safety of their hospital community throughout the COVID-19 pandemic and how they navigated the particular difficulties of their roles. I had a unique vantage point as a student and visitor to the community to see common struggles and challenges across the hospital, and I recognized through the interview process that these hardships are too often experienced in isolation.
“I was reminded of the importance of valuing everyone’s unique and important contribution within a system that can, at times, be fragmented. It was an honor to bear witness to the stories shared by my interviewees. As I move through various hospitals and communities in my training as a medical student, I hope to carry the lesson of recognizing each individuals’ humanity beyond their job title—whether it may be a nurse, security manager, respiratory therapist or infection control specialist.”
Charting Crisis: Collective Storytelling in an Age of COVID-19
Since the spring of 2020, the National Humanities Center’s COVID-19 Oral History Project has trained students to collect the personal stories and experiences of healthcare workers whose lives have been profoundly affected by the pandemic. By curating, archiving, and sharing these narratives, the NHC will help to facilitate conversations about important contemporary issues in our health systems and in our broader society.
